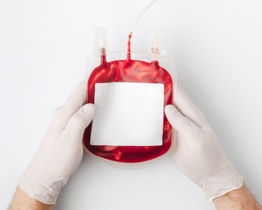
ABOUT BLOOD SAFETY
The blood supply in the United States is much safer today than ever before. The Food and Drug Administration (FDA) regulates collection and testing of the blood supply. The FDA inspects organizations that collect blood to make sure that they are following the regulations. Thanks to modern safeguards, it is more likely to die from a lightning strike than to get an HIV or hepatitis infection from a blood transfusion. These measures are in place to decrease the risk of infection in the blood supply:
- Questions that identify potential donors at risk for infection
- Physical examination of the donor
- Strict donation procedures using sterile supplies
- Testing for HIV, hepatitis B, hepatitis C and several other infections
Prior to donation, a donor answers thorough questions about behavior and travel in a confidential setting, which encourages honest answers. The donor then goes through a limited physical exam in which the donor’s temperature is taken to make sure that the donor does not have a fever. Potential donors found to be at risk for infection due to their answers to the questions or due to their temperature are not allowed to donate blood.
The blood is collected using sterile, single use supplies and then a sample of blood is tested for infection. Blood showing evidence of disease is discarded and the donor is not allowed to make future donations.
BLOOD TYPES
Your blood type determines what type you can receive and which type of donation you’re encouraged to make.
A-
A-: A person with type A- blood can donate to a person with type A or type AB blood and can receive blood from a person with type A- or type O- blood. If you have the A- blood type, you are encouraged to donate whole blood or double red cells.
B-
B-: This blood type is one of the rarer blood types and can only receive O- and B- blood. If you have B- blood, you are encouraged to donate double red cells or whole blood.
O-
O-: As the universal red cell donor, O- is transfused into any patient needing this life-saving gift. It is the blood type in greatest demand. Making up only 6.6% of the population, O- blood is one of the most precious gifts anyone can give. A single trauma can quickly deplete the community’s supply. Donors with O- blood type are encouraged to give double red cells and whole blood.
AB-
AB-: Individuals with AB- blood type have the potential to save anyone. AB- platelet and plasma can be transfused into any person, regardless of their blood type.This is the rarest blood type, making up less than 1% of the population.
A+
A+: This blood type makes up 35.7% of the population. People with A+ blood type are encouraged to donate platelets, whole blood or double red cells.
B+
B+: A person with type B+ blood can receive type B or type O blood only. Donors with this blood type are encouraged to donate platelets and plasma.
O+
O+: This blood type is the most common blood type, making up more than 37.4% of the population. Any positive blood type can receive O positive blood. Donors with this blood type are encouraged to give double red cells and whole blood.
AB+
AB+: AB+ plasma can be given to any patient and is in extremely high demand. Plasma is often used for trauma or burn victims. AB+ platelets can also be given to patients of many different blood types. Platelets are the cells that help make clots and are given to patients being treated for cancer or to patients who are having surgery or another procedure.
FREQUENTLY ASKED QUESTIONS
There are many reasons you might need a blood transfusion. You may need a transfusion because of the effect a disease, surgery, chemotherapy, or other treatments have on your blood. Your doctor can explain why you need a transfusion.
If you and your doctor decide you need a transfusion then you may be given one or more of the following blood products, red blood cells, white blood cells, platelets, plasma or cryoprecipitate.
- You may need a transfusion of red blood cells if you have a low blood count or hemoglobin and are symptomatic(anemic). This is common if you have had bleeding due to trauma, surgery, or cannot make enough red blood cells for example due to cancer treatment.
- You may need a platelet transfusion if your platelet count is low (thrombocytopenia) and you are at risk for bleeding.
- You may need a transfusion of plasma, this happens most frequently in times of major surgery or significant blood loss due to trauma.
- You can also have a white blood cell transfusion, but these are rare and done only in very specific situations.
Don’t be afraid to ask your doctor why you need blood. Your care provider should be able to tell you the reason you need a transfusion and what sort of blood or blood products you may need.
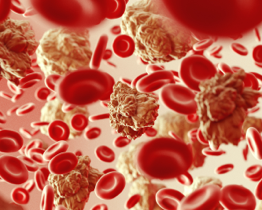
A blood component is any part of the blood that is transfused (given) to a patient. Blood donors can donate whole blood or specific components such as red cells, plasma and platelets. Whole blood is usually separated into different components such as red cells, plasma and platelets at a blood center.
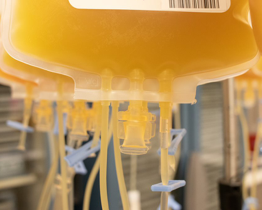
When you come to donate a unit of blood, that unit is not kept in its whole blood form. The unit is centrifuged at high speeds to separate the constituent components from each other. Since red blood cells are the heaviest, they sink to the bottom of the bag. The platelet rich plasma and cryoprecipitate factors settle near the middle of the bag. Each of these components are separated into different bags for treatment as follows:
Red Blood Cells: Used to increase red cell mass after surgery, to treat patients with anemia. Red cells are stored under refrigeration for up to 42 days, or they may be frozen for up to 10 years.
Fresh Frozen Plasma: Used to treat clotting disorders, expand blood volume, to treat shock due to plasma loss in burns. FFP is frozen shortly after collection and is stored up to one year.
Platelets: Used to treat bleeding due to platelet shortage or to treat platelet function abnormalities. Platelets are stored at room temperature with constant agitation for up to 5 days.
Cryoprecipitate: Used to treat Hemophilia A, Von Willebrand’s disease, and other clotting factor deficiencies. Cryo is made from FFP and may be stored frozen up to one year.
White Blood Cells: Used to treat patients who cannot produce enough white cells, due to disease or cancer treatment or are unresponsive to antibiotic therapy. They must be transfused within 24 hours after collection.
Immune Globulin: Given to help fight infectious diseases such as hepatitis.
Albumin: Used to treat people in shock, and also used in plasma exchanges for seriously ill patients.
One unit of whole blood can help save as many three lives.
It doesn’t hurt to have a blood transfusion. Most of the time it requires a needle with an intravenous line be started in your arm. The only pain you may feel is when the needle is placed into your vein. This pain will go away quickly.
If you have a central venous catheter (CVC), you can get red blood cells or platelets through it. This will not hurt.
If you have a Mediport®, it will be the same type of needle stick that you have for chemotherapy.
Your blood type is either A, B, AB, or O. It’s either Rh positive (+) or Rh negative (-). Before you receive a transfusion of red blood cells your blood will be tested for ABO and Rh as well as a screen for unexpected antibodies to red blood cells.
Your blood type will be checked with a test called a type and crossmatch or type and screen. The results of these tests are used to match your blood type with the blood in the blood bank. Prior to starting the blood transfusion your healthcare provider will check to make sure that the blood is the correct match for you before they give you the transfusion. Some products such as platelets do not need to be ABO matched and others, such as plasma do not need to be matched exactly but must be compatible.
There is a very rigorous process put in place to ensure that you get safe blood of the right blood type and right unit of red blood cells. First, multiple steps in the lab and at the bedside will be taken to confirm your identify during the process. If you need a type and cross match, a blood sample will be needed. When your blood sample is drawn, the tubes will be labelled with your information in your presence. This testing is done to ensure the units you will receive are compatible with your blood. The testing of your blood type will be done by at least two different people or will be compared to your previous results. When the initial sample is collected for typing and cross matching you will have a bracelet put on your arm that links you to the specimen drawn. It is important to keep than arm band in place and notify your healthcare provider if it is removed for any reason.
Once the blood is ready, the blood product will be checked again at your bedside. Your health care provider may ask you to state your name and date of birth. They will also check the label carefully against the details of your identification band and/or chart.
There are several factors that determine how long it will take for your transfusion to begin. These include:
If your blood has not been tested for your blood type recently, and you need red cells, a type and crossmatch will need to be done. (There are rules about far in advance this test can be performed) and may take 2 to 4 hours to be processed in the blood bank. It may take longer if additional antibodies are found in your blood or if your immunotherapy medications affect your test results.
For platelets, plasma and cryoprecipitate only an ABO typing will be needed.
The timing also depends on where the blood you need is stored. If you have a rare blood type or antibody, blood may not be available in your hospital and may have to be ordered from the local blood center or another blood center.
It is important to note that if you need blood urgently, hospitals have systems in place to support this need.
The blood will be transfused intravenously (IV), which means to will go into your vein via a tube usually in your arm. The blood is in a bag that is attached to the tubing.
Your temperature, pulse and blood pressure will be tested before the procedure begins and then again during the transfusion and again at the end.
One transfusion of red blood cells usually takes 2 to 4 hours. One transfusion of platelets takes 30 to 60 minutes. One transfusion of plasma usually takes 20 to 30 minutes. Blood can be transfused as fast your body will tolerate. Your physician will determine how fast this is and a nurse will monitor that you are okay during the transfusion. Someone will come back to check on you several times during your transfusion.
Your health care provider will check on you during the transfusion. Your temperature, pulse and blood pressure will be tested before the procedure begins and then again during the transfusion and again at the end. If you do not feel well at any time during the transfusion, be sure to tell your health care provider.
You may feel normal or you may experience some side effects. Side effects are not very common but could happen during or after your transfusion. They may include:
Shortness of breath
Rash or hives
Hot flashes or chills
Nausea and/or vomiting
Back pain
Light headedness or dizziness
If you experience any of these symptoms or anything unusual during or after your transfusion, be sure to tell your health care provider.
Even with all the precautions and testing, blood transfusions, like all medical procedures still have some risks. These risks include the very small chance (less than 1 in 100) of having an allergic reaction, shortness of breath or a rash/hives. In extremely rare cases, you may get an infection. Your healthcare provider will talk with you about these risks before you receive a transfusion.
There are many safeguards in place in the United States to ensure a safe blood supply. Before donating blood, all donors must complete a confidential interview and health check. After blood is donated, the blood is tested for blood type (ABO and Rh), antibodies and is screened for infectious diseases including:
- Syphilis
- Hepatitis B and C
- HIV
- A virus associated with a very rare form of leukemia
- West Nile virus
- Trypanosoma cruzi (a parasite that causes Chagas disease)
- Zika virus
- Bacteria (platelets only)
If the donated blood tests show any of these infections, the blood is discarded and not used.
Yes, it is possible for friends and relatives to donate both red blood cells and platelets. These are called directed donations. These donations are tested in the same way as other donations. This must be arranged in advance of your surgery. If the blood tests positive for any of the viruses listed above, the donor will be notified privately.
If your friend or relative’s blood type isn’t the same as your blood type, the donation may be given to someone else who may need it.
Even though directed donations are possible, they are not recommended by most transfusion experts and many times there is an additional fee for this. There is no proof that directed blood is any safer than other donated blood. In fact related donors may pose the risk of transfusion associated graft versus host disease and require additional steps (irradiation of the unit) to reduce this risk. Asking someone for a directed donation may put the donor in an uncomfortable situation and may compromise the reliability of the donor’s answers to the health questions.
Volunteer blood is safe. However, in some instances, such as a patient with many antibodies or compatibility issues, health care providers may encourage people scheduled for surgery to donate their own blood. The blood is stored and given back if and when you need it. This is called an autologous donation.
Ask your doctor if you can donate your own blood. If this is possible, arrangements will be made with the blood bank for you to begin banking your blood. In order to do this, you will need enough time to restore red cells before surgery. You may donate your own blood several times before your surgery and your red cell count will be tested before each donation to make sure the donations are not making you anemic. Your blood is good for 42 days. For more information about autologous blood donations, read the resource Being Your Own Blood Donor.
It’s always your right to refuse a treatment. However, keep in mind that doctors recommend a transfusion only when they think it is needed. A large amount of blood is lost during some types of surgery. If this blood is not replaced, you can die.
If you want to avoid a blood transfusion or want to reduce the amount of blood you will need, it is important to talk to your doctor about this as early in the process is possible.
If you are a Jehovah’s Witness or have other objections to blood transfusion, it is important to discuss this with your doctor.
There are no substitutes for blood. This is why we are so grateful to the many family members and friends who donate their blood.
If you are anemic (have a low blood count) you can discuss with your doctor how to increase your blood count by other ways.
A blood transfusion can sometimes cause reactions. The most common symptoms are an increase in temperature, chills, and hives. These can be treated with medication. Transfusion reactions are rarely life-threatening. Your nurse will monitor you carefully while your blood transfusion is taking place.
- An elevation in temperature
- Chills
- Redness and warmth in your face
- Hives, rash, or itching
- Trouble breathing or shortness of breath
- Lower back pain
- Nausea or vomiting
- Weakness or fainting
- Dark-colored urine (pee)
If you have chest pain, call 911 right away. After your transfusion follow the list of instructions given to you.
What is COVID-19 convalescent plasma?
When a person has a virus such as COVID-19, their immune system creates antibodies to fight the virus. Those antibodies are found in plasma, which is the liquid part of blood. Plasma with these infection-fighting antibodies is called “convalescent plasma.” Through a blood donation process, plasma can be collected from a recovered person, then transfused to a sick patient who is still fighting the virus. This provides a boost to the immune system of the sick patient and may help speed the recovery process.
The FDA has identified use of COVID-19 convalescent plasma as an important investigational treatment for patients with moderate or severe illness due to COVID-19. You will also see COVID-19 convalescent plasma referred to as COVID plasma or CCP. CCP is considered an investigational treatment because clinical studies are underway but have not yet been completed. We know there is evidence that CCP has helped patients with other illnesses. Doctors and researchers are currently working on studies to determine how effective COVID plasma will be in treating COVID-19 patients.
For more information about COVID-19 convalescent plasma visit this website: https://covidplasma.org/#what_is_convalescent_plasma